What the Da Vinci Surgical System Actually Does — And Why It Matters for Women
Categories:
By: Ethan Cole
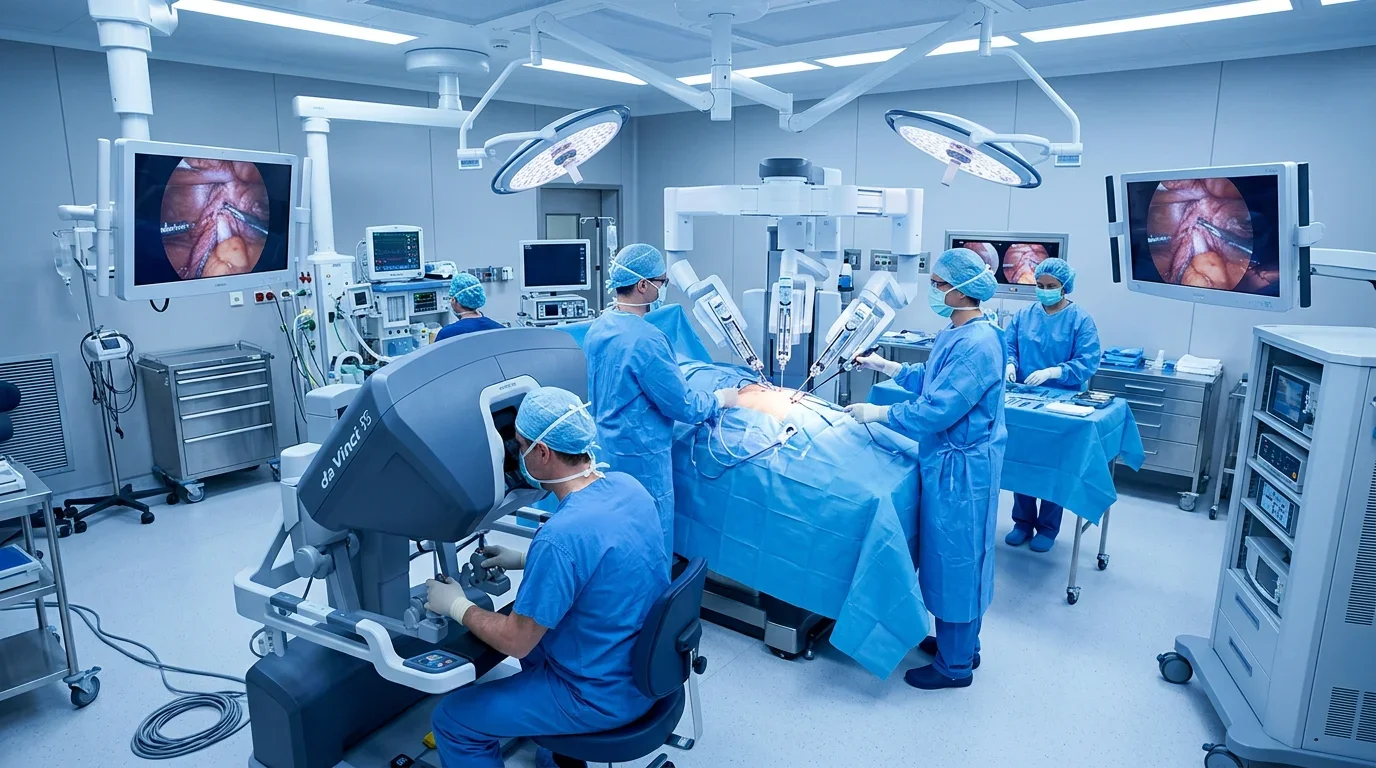
The da Vinci Surgical System is a robotic platform that allows surgeons to perform complex procedures through a few tiny incisions rather than a large abdominal opening. It gives the surgeon enhanced vision, finer instrument control, and a steadier hand than traditional surgery allows — which translates to less tissue damage, faster recovery, and better outcomes for patients.
If you've been told you need gynecologic surgery — or you're exploring options for a procedure like tubal reversal — you've probably come across the term "da Vinci" more than once. Most explanations stop at "it's a robot." That's not particularly helpful when you're trying to decide whether this approach is right for you.
This is a plain-language breakdown of what the da Vinci Surgical System actually does, how it differs from conventional surgery, and why the distinction matters specifically for women's gynecologic procedures. If you're considering robotic gynecologic surgery with Dr. Neef, start here.
What the Da Vinci System Is (And What It Isn't)
The da Vinci is not an autonomous robot. It doesn't make decisions or operate independently. It's a precision surgical tool — an extension of the surgeon's hands — that translates the surgeon's movements into smaller, more controlled actions inside the body. The surgeon drives everything; the system just makes those movements more precise.
This is the misconception that stops a lot of patients cold. "A robot is doing my surgery" sounds alarming. The reality is more like: your surgeon is performing your surgery using an instrument that dramatically improves what they can see and do.
Here's how the system actually works:
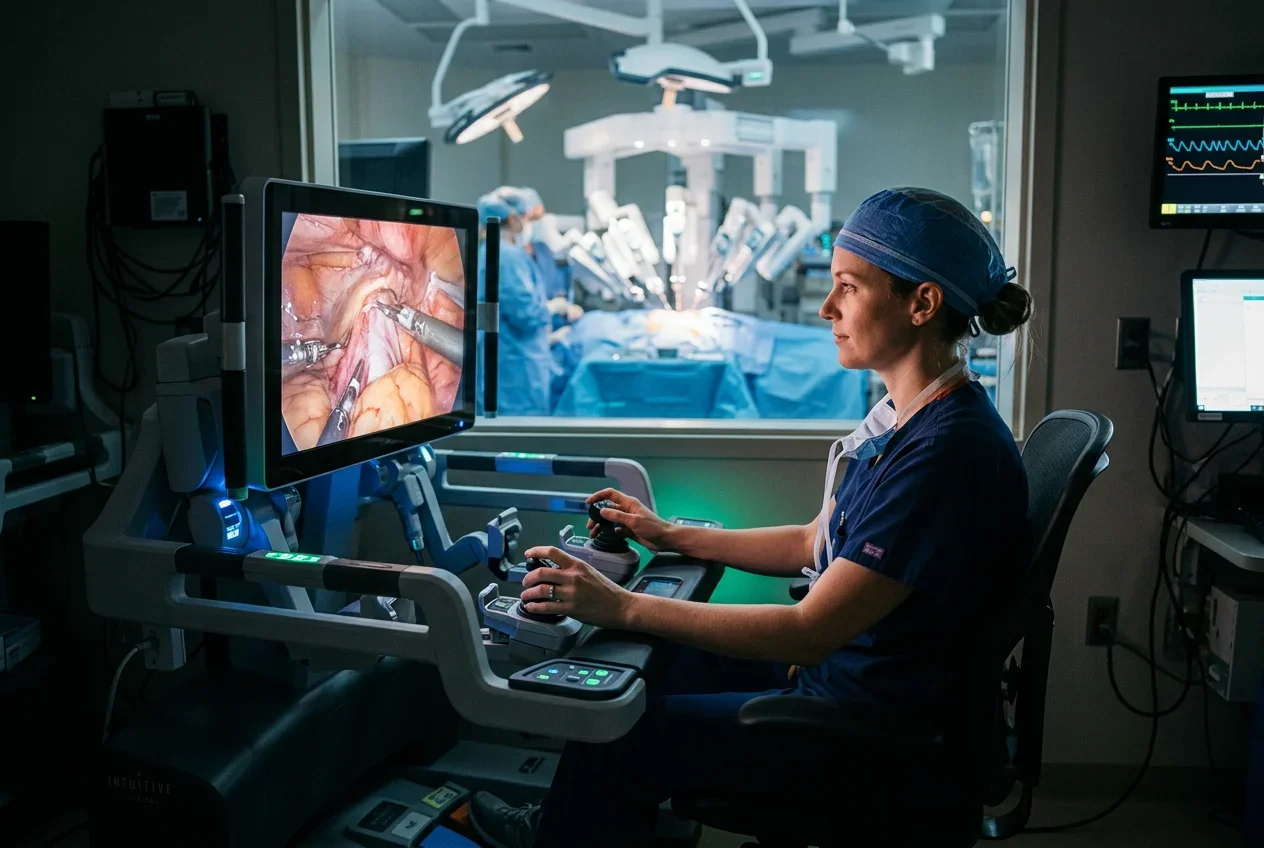
The surgeon sits at a console a few feet from the operating table, viewing a magnified 3D image of the surgical site
The surgeon's hand movements are captured and translated in real time to instrument tips inside the patient's body
The instruments move at a reduced scale — large hand movements become small, precise instrument actions
Tremor is filtered out — the system removes natural hand tremor that would otherwise affect instrument steadiness
Four robotic arms hold the instruments and a camera through small incisions (typically 1–2 cm each)
What the system doesn't do: it doesn't plan the surgery, adjust for complications, or make any judgment calls. That's entirely the surgeon's role.
|
Feature |
Traditional Open Surgery |
Laparoscopic Surgery |
Da Vinci Robotic Surgery |
|
Incision size |
4–8 inches |
3–4 small ports |
3–4 tiny ports (1–2 cm) |
|
Surgeon's view |
Direct, magnified loupe |
2D camera on monitor |
3D magnified HD camera |
|
Instrument range of motion |
Full hand movement |
Limited pivot range |
540° wristed movement |
|
Tremor control |
None |
None |
Filtered by system |
|
Surgeon position |
Standing over patient |
Standing, awkward angles |
Seated at console |
Why Precision at This Scale Matters for Gynecologic Surgery
Gynecologic procedures often involve delicate structures — fallopian tubes, ovarian tissue, the uterine wall — where the margin between a clean repair and unnecessary damage is measured in millimeters. The da Vinci system's magnification and instrument dexterity give surgeons the ability to work at a level of precision that traditional tools simply don't allow.
The fallopian tubes are a good example. Each tube is roughly the diameter of a piece of spaghetti. Tubal reversal surgery requires suturing the two cut ends back together with thread finer than a human hair. That's not a metaphor — it's a real description of microsurgical technique. At that scale, even slight instrument shake or limited visibility significantly affects the outcome.
What 3D Magnification Changes
Standard laparoscopic surgery uses a 2D camera. Surgeons have long adapted to working without depth perception, but it's a real limitation — especially for precise suturing. The da Vinci's 3D HD camera restores natural depth perception at 10x magnification, which means the surgeon can judge distances accurately at a microscopic scale.
What Wristed Instruments Change
Conventional laparoscopic instruments pivot at the point of entry into the body. This limits range of motion and requires the surgeon to work at counterintuitive angles. Da Vinci instruments have a wrist joint at the tip — they can rotate and articulate in any direction, mimicking the range of a human wrist but in a much smaller space.
For gynecologic procedures, this means the surgeon can work around structures, angle sutures correctly, and access tight spaces without repositioning instruments or enlarging incisions.
|
Procedure Type |
Why Da Vinci Precision Matters |
|
Tubal reversal |
Microsurgical suturing of 1–2mm tubal diameter |
|
Myomectomy (fibroid removal) |
Precise excision preserving uterine wall integrity |
|
Hysterectomy |
Reduced blood loss, cleaner tissue planes |
|
Endometriosis excision |
Fine dissection around nerves and bowel |
|
Ovarian cystectomy |
Preservation of healthy ovarian tissue |
Key Takeaways
The da Vinci is a surgical tool, not an autonomous robot. The surgeon controls every movement; the system amplifies precision.
3D magnification restores depth perception at up to 10x magnification — a significant advantage over 2D laparoscopic cameras.
Wristed instrument tips mimic the human wrist with greater range than conventional laparoscopic tools allow.
Tremor filtering removes natural hand shake, which matters most in microsurgical procedures like tubal reversal.
Smaller incisions mean less tissue trauma — which directly shortens recovery and reduces infection risk.
Surgeon experience still drives outcomes. The da Vinci system enhances skill; it doesn't replace it.
What This Means for Your Recovery
Because da Vinci procedures are performed through small incisions rather than large abdominal openings, patients typically experience less post-operative pain, shorter hospital stays, and faster returns to normal activity compared to open surgery. For many gynecologic procedures, patients go home the same day.
Recovery after robotic gynecologic surgery differs meaningfully from what patients experience after traditional open procedures. Here's what's different and why:
Less blood loss. Smaller incisions and precise tissue handling reduce intraoperative bleeding, which affects how patients feel in the days following surgery.
Less pain. Muscle tissue isn't cut to create access the way it is in open surgery. Most patients manage post-operative discomfort with over-the-counter medication.
Lower infection risk. Smaller openings mean less exposure of internal tissue to external environment.
Faster return to normal activity. Most robotic surgery patients resume desk work and light activity within 1–2 weeks. Open surgery typically requires 4–6 weeks before similar milestones.
Less visible scarring. Tiny port incisions leave minimal marks compared to a full abdominal incision.
Here's what that typically looks like across common gynecologic procedures:
|
Procedure |
Open Surgery Recovery |
Robotic Surgery Recovery |
|
Tubal reversal |
4–6 weeks |
1–2 weeks |
|
Hysterectomy |
6–8 weeks |
2–4 weeks |
|
Myomectomy |
4–6 weeks |
2–3 weeks |
|
Endometriosis excision |
3–5 weeks |
1–2 weeks |
Recovery time is a real-world number that affects childcare, work, and daily logistics. For most women, cutting recovery in half isn't a minor convenience — it's a significant factor in how feasible surgery feels.
Conclusion
The da Vinci Surgical System matters because it closes the gap between what a surgeon intends to do and what their instruments can actually execute. Better vision, steadier instruments, and greater range of motion — in surgeries where millimeters matter, those advantages compound into meaningfully better outcomes for patients.
For gynecologic procedures especially, the da Vinci's precision supports cleaner repairs, preserved tissue, and the kind of recovery that fits into a real life. If you're exploring robotic surgery options in the DFW area and want to understand whether this approach fits your specific procedure,contact Dr. Neef's office to schedule a consultation.
Ready to learn if robotic surgery is right for you? Schedule a consultation with Dr. Neef today.
Call (817) 568-8731Categories:
Frequently Asked Questions
-
No. The da Vinci system has no autonomous capability. Every movement is directed by the surgeon in real time from a console. The system translates those movements into precise instrument actions — the surgeon is fully in control throughout.
-
Most robotic procedures use 3–4 small incisions, typically 1–2 cm each. This is comparable to standard laparoscopic surgery and significantly smaller than open surgical incisions.
-
Not all procedures require or benefit equally from robotic assistance. It's most advantageous for procedures requiring fine suturing, precise tissue dissection, or work in tight anatomical spaces — like tubal reversal, hysterectomy, myomectomy, and endometriosis excision.
-
Robotic surgery reduces certain risks associated with large incisions — blood loss, infection, and tissue trauma. Overall safety depends on many factors including the surgeon's experience, patient health, and procedure complexity. Discuss your specific risk profile with your surgeon.
-
Procedure time varies by surgery type and complexity. Most robotic gynecologic procedures take 1–3 hours. Surgeon experience with the robotic platform also affects efficiency.
-
No. Recovery sensation is related to incision size, tissue handling, and the extent of the procedure — not whether robotic instruments were used. Most patients report less discomfort after robotic procedures compared to open surgery.
-
Yes. The system includes tremor filtration that removes natural hand shake from the surgeon's movements before translating them to the instrument tips. This is particularly relevant for microsurgical procedures.
-
No. Surgeons require specific credentialing and training to operate the da Vinci system. Experience level matters — surgeons who perform robotic procedures regularly achieve better outcomes than those who use the platform infrequently.
-
Standard laparoscopic cameras produce a 2D image on a flat monitor, which eliminates depth perception. The da Vinci uses a dual-lens camera system to produce a true 3D high-definition image that restores natural depth perception at up to 10x magnification.
-
Yes. Dr. Jason Neef performs robotic gynecologic procedures — including tubal reversal, hysterectomy, and other minimally invasive surgeries — at Texas Health Huguley in the DFW area. Contact the office to discuss your specific procedure.
Texas Health Huguley Hospital
Fort Worth South Medical Office Building 3