Robotic Gynecologic Surgery: How Da Vinci Technology Transforms Women's Health
Categories:
By: Ethan Cole
Robotic gynecologic surgery uses the Da Vinci surgical system to perform complex women's health procedures through tiny incisions, giving your surgeon enhanced 3D visualization, microsurgical precision, and range of motion that traditional techniques can't match. The result: less pain, smaller scars, faster recovery, and better outcomes for procedures like tubal reversal, Essure reversal, and hysterectomy.
Whether you're considering a robotic surgical procedure to restore your fertility or resolve chronic gynecologic pain, the technology behind it matters. Robotic-assisted laparoscopy represents the most advanced approach to women's surgical care available today — and understanding how it works helps you make confident decisions about your treatment.
This guide covers the full picture: how the Da Vinci system actually works during gynecologic procedures, which surgeries benefit most from the robotic approach, what the evidence says about outcomes, and what your experience will look like from consultation through recovery.
How Does the Da Vinci Robotic Surgical System Work for Gynecology?
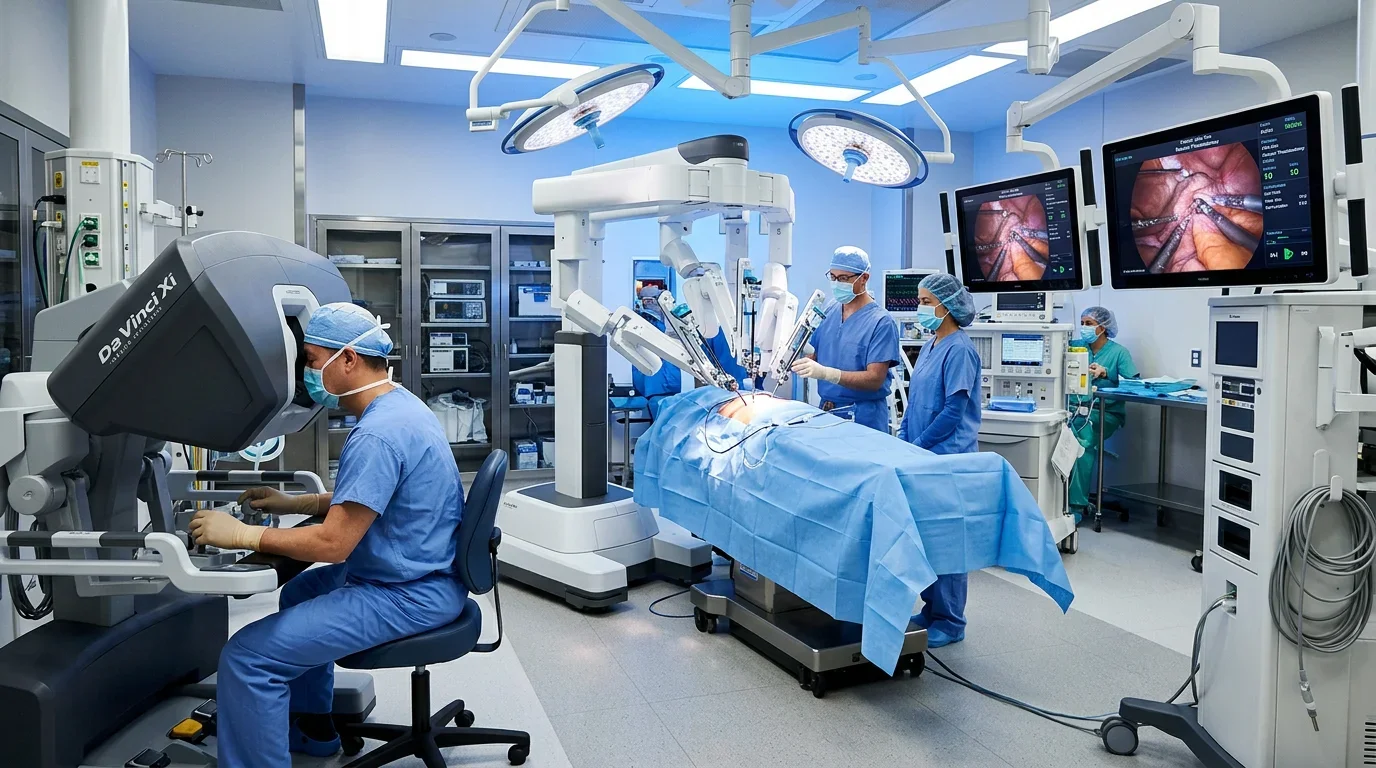
The Da Vinci system consists of three components: a surgeon console where your doctor sits and controls the surgery, a patient-side cart with robotic arms that hold surgical instruments, and a vision tower providing magnified 3D high-definition views of the surgical field. Your surgeon is always in complete control — the robot doesn't operate autonomously.
Let's clear up the biggest misconception right away. The word "robot" makes people think a machine is performing their surgery. That's not how it works. The Da Vinci system is a tool — controlled entirely by your surgeon's hands and eyes. Every movement of the robotic arms is a direct translation of your surgeon's hand movements at the console. Think of it like power steering in a car: the technology amplifies and refines what the driver does, but the driver is always in charge.
Your surgeon sits at an ergonomic console positioned near you in the operating room. Looking through a binocular viewpiece, they see your internal anatomy in magnified three-dimensional high definition — far more detail than the naked eye or a standard laparoscopic camera provides. Their fingers control master manipulators that translate movements to the robotic arms in real-time.
The robotic arms hold EndoWrist instruments — tiny surgical tools with wrist-like joints that bend and rotate with greater range of motion than the human wrist. This wristed capability is one of the most significant advantages over standard laparoscopy, where instruments are straight and rigid. For delicate gynecologic procedures like robotic laparoscopic surgery on fallopian tubes, this extra articulation makes a real difference in surgical precision.
The system also features built-in motion scaling and tremor filtration. Motion scaling means your surgeon can make a one-inch hand movement that translates to a precise quarter-inch movement at the instrument tip. Tremor filtration eliminates the tiny natural vibrations in human hands. Together, these features enable microsurgical work that would be extremely difficult — or impossible — by hand alone.
|
System Component |
What It Does |
Patient Benefit |
|
Surgeon Console |
Surgeon controls all movement via hand manipulators |
Surgeon has optimal ergonomics for focus and precision |
|
Patient-Side Cart |
Robotic arms hold instruments and camera inside your body |
Small incisions (5-12mm), minimal tissue disruption |
|
3D HD Vision |
Magnified three-dimensional view of surgical field |
Surgeon sees anatomy in greater detail than open surgery |
|
EndoWrist Instruments |
Wristed tools with 7 degrees of freedom |
Access tight spaces with greater dexterity than hand alone |
|
Motion Scaling |
Translates large hand movements into micro-movements |
Ultra-precise suturing and tissue handling |
|
Tremor Filtration |
Removes involuntary hand tremors |
Smoother, more controlled instrument movements |
Which Gynecologic Procedures Benefit Most from Robotic Surgery?
The robotic approach provides the greatest advantage for procedures requiring microsurgical precision in tight anatomical spaces — particularly tubal reversal, Essure reversal, and hysterectomy. Dr. Jason Neef, MD, is the only surgeon in the DFW area performing all three of these procedures on the Da Vinci platform.
Not every gynecologic surgery requires the robotic approach, but the procedures that benefit most share common characteristics: they involve delicate tissue handling, precise suturing, or work in confined pelvic spaces where the enhanced visualization and wristed instruments of the Da Vinci system make a measurable difference in outcomes.
Robotic Tubal Reversal. This is where the precision of the Da Vinci system shines brightest. Reconnecting fallopian tubes requires microsurgical sutures finer than a human hair, placed with millimeter accuracy. The 3D magnification and tremor-free robotic movements allow your surgeon to preserve maximum tube length — directly impacting your pregnancy success rates. Women considering tubal ligation reversal surgery benefit significantly from the robotic approach because less internal scarring means a better environment for egg and sperm to meet.
Robotic Essure Reversal. Removing Essure devices and reimplanting the fallopian tubes into the uterus is one of the most technically demanding gynecologic procedures. It requires resection of the uterine cornua (corner), extraction of the coil and scar tissue, and careful tube reimplantation. Only a handful of surgeons nationally perform this robotically — Dr. Neef is one of them. The robotic platform's precision is essential for this highly specialized Essure reversal procedure.
Robotic Hysterectomy. Whether indicated for fibroids, endometriosis, abnormal bleeding, or other conditions, a robotic laparoscopic hysterectomy typically means same-day discharge, a two-week recovery, and significantly less pain than an abdominal approach. The robotic platform gives the surgeon superior visibility inside the pelvis, which is particularly valuable for complex cases involving adhesions or large uterine fibroids.
|
Procedure |
Why Robotic Excels |
Key Advantage |
Typical Recovery |
|
Tubal Reversal |
Microsurgical reconnection of fallopian tubes |
3D magnification for hair-thin suturing |
~1 week |
|
Essure Reversal |
Cornual resection + tube reimplantation |
Wristed instruments for tight uterine corners |
~2 weeks |
|
Hysterectomy |
Complete uterus removal through small incisions |
Superior pelvic visualization |
~2 weeks |
|
Myomectomy |
Fibroid removal preserving the uterus |
Precise dissection minimizing blood loss |
~2 weeks |
|
Endometriosis Excision |
Removal of deep infiltrating tissue |
Enhanced visualization of disease extent |
~1-2 weeks |
Beyond these core procedures, the robotic platform is increasingly used for ovarian cyst removal, pelvic prolapse repair, and other gynecologic conditions where the minimally invasive approach improves outcomes.
What Are the Proven Benefits of Robotic Over Traditional Gynecologic Surgery?
Research consistently shows robotic gynecologic surgery results in less blood loss, fewer complications, shorter hospital stays, faster recovery, and smaller scars compared to traditional open abdominal surgery. Robotic procedures also offer advantages over standard laparoscopy for complex cases requiring microsurgical precision.
The benefits aren't theoretical — they're backed by clinical data and the lived experience of thousands of patients. According to the American College of Obstetricians and Gynecologists (ACOG), minimally invasive approaches should be the preferred method for gynecologic surgery when technically feasible, and robotic assistance extends that feasibility to more complex procedures.
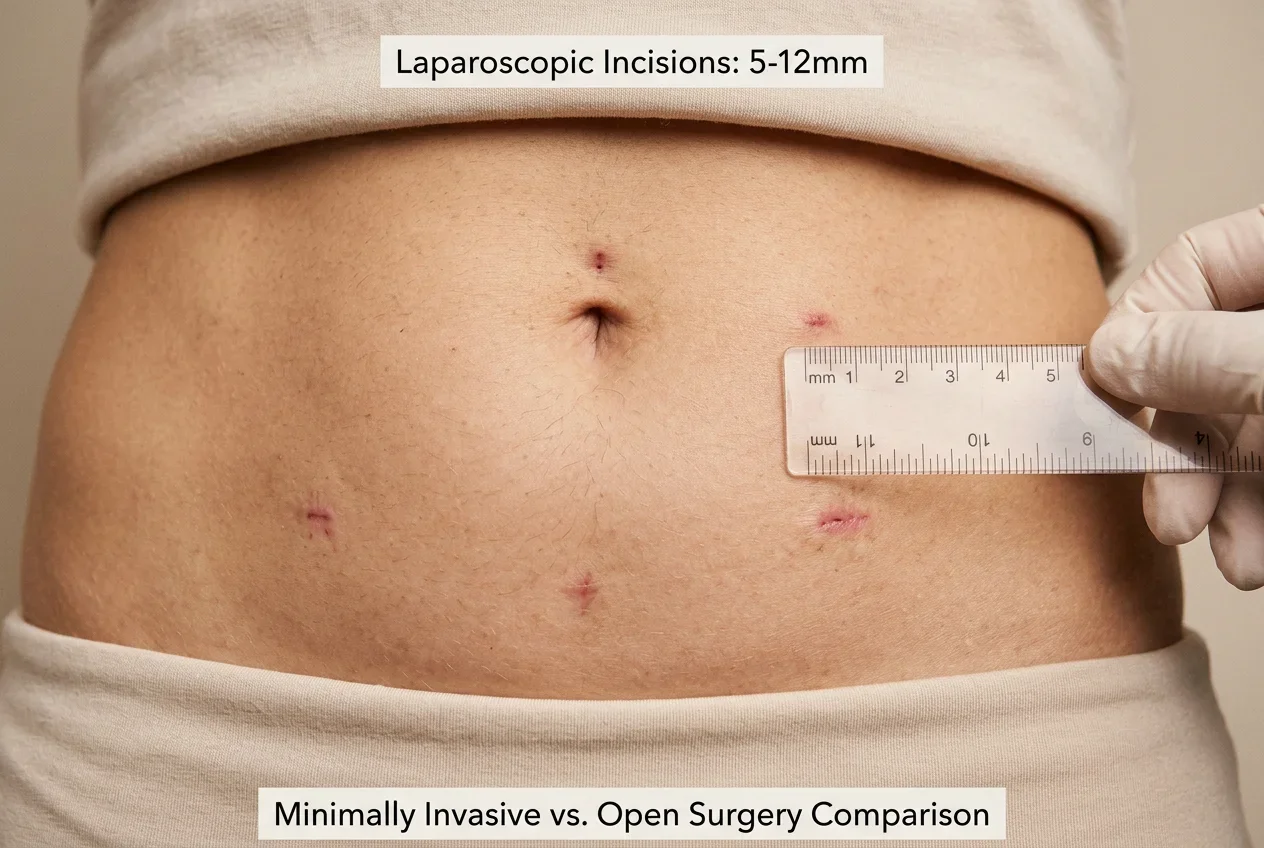
Here's what the evidence tells us about specific outcomes. Blood loss during robotic hysterectomy is typically measured in tablespoons rather than the cups sometimes seen with open surgery. Surgical site infection rates drop significantly because the incisions are so small — 5-12mm ports versus a 4-6 inch abdominal cut. Hospital stays shrink from two to three days down to same-day discharge for many robotic procedures. And the big one patients care about most: recovery time drops from four to six weeks to approximately one to two weeks.
The cosmetic benefit matters to patients too, even if it's rarely the primary reason for choosing robotic surgery. Four or five tiny incision marks that fade to nearly invisible over time versus a prominent abdominal scar — it's a meaningful quality-of-life difference for many women.
There's also a less obvious benefit: reduced adhesion formation. Internal scar tissue (adhesions) after surgery can cause chronic pain, bowel obstruction, and fertility problems. Because the robotic laparoscopic surgeon works through minimal incisions with minimal tissue handling, the inflammatory response is lower and adhesion formation is reduced. For fertility procedures like tubal reversal, this directly impacts pregnancy success.
|
Outcome Measure |
Robotic Approach |
Open Abdominal Approach |
|
Incision Size |
4-5 ports, 5-12mm each |
4-6 inch single incision |
|
Average Blood Loss |
Minimal (tablespoons) |
Moderate to significant |
|
Infection Risk |
Lower (small incisions) |
Higher (large wound) |
|
Hospital Stay |
Same day to 1 night |
2-3 days typical |
|
Return to Work |
1-2 weeks |
4-6 weeks |
|
Internal Scarring |
Reduced adhesion formation |
Higher adhesion risk |
|
Surgical Success Rate |
90-96% across procedures |
Comparable, but with more complications |
Sound familiar? If your current doctor recommended an open abdominal approach and you're wondering whether a minimally invasive gynecologic surgery option exists — it very likely does. Not every surgeon has robotic training, so the approach offered to you may depend more on your surgeon's skillset than on what's actually best for your situation.
Key Takeaways
The Da Vinci system is surgeon-controlled — your doctor directs every movement through a console with 3D magnified vision and robotic precision. The robot never operates on its own.
Robotic gynecologic surgery excels for tubal reversal, Essure reversal, and hysterectomy because these procedures require microsurgical precision in confined pelvic spaces.
Recovery is dramatically faster — most patients return to normal activities in one to two weeks compared to four to six weeks for open surgery.
Smaller incisions mean less pain, less scarring, and fewer complications including reduced infection risk and lower adhesion formation that can impact future fertility.
Dr. Neef is the only DFW surgeon performing all three core robotic gynecologic procedures (tubal reversal, Essure reversal, hysterectomy) on the Da Vinci platform.
Clinical evidence supports the robotic approach for better outcomes across blood loss, hospital stay, complication rates, and return-to-work timelines.
What Should You Expect from Your Robotic Gynecologic Surgery Experience?
Your experience begins with a thorough consultation where Dr. Neef reviews your medical history, performs an exam, and discusses your treatment options. Surgery day at Texas Health Huguley Hospital in Burleson includes concierge-level service from valet check-in through discharge, with most robotic procedures taking one to three hours and many patients going home the same day.
The patient experience at Dr. Neef's practice is intentionally different from what you might expect at a large Dallas or Fort Worth medical center. Texas Health Huguley is a community hospital that delivers big-city expertise without the big-city hassle — no traffic headaches, no parking garages, no impersonal waiting rooms. Valet parking, a dedicated surgical team, and personalized attention define the experience from start to finish.
Your journey starts with a preoperative consultation one to fourteen days before surgery. During this visit, you'll undergo a physical exam, pelvic ultrasound, and bloodwork. Dr. Neef personally reviews your medical and surgical history, discusses your goals, and creates a surgical plan tailored to your specific anatomy and condition. For fertility procedures, he'll review your previous tubal ligation records and your partner's semen analysis.
On surgery day, you'll arrive at the hospital and be prepped for general anesthesia. The procedure itself typically takes one to three hours depending on complexity. Dr. Neef sits at the Da Vinci console while a surgical assistant is positioned at your side throughout the procedure. After surgery, you'll recover in the post-anesthesia care unit before being evaluated for discharge.
Most patients undergoing robotic surgery go home the same day or after an overnight stay. You'll leave with clear discharge instructions, a prescription for pain medication (though many patients transition to over-the-counter NSAIDs within 48-72 hours), and a follow-up appointment scheduled. Dr. Neef's team is available by phone if any questions come up during your recovery.
Explore your robotic gynecologic surgery options with Dr. Neef. Contact us today to schedule your consultation — expert care, close to home.
Call (817) 568-8731Categories:
Frequently Asked Questions
-
Your surgeon controls every single movement. The Da Vinci system is a tool that translates your surgeon's hand movements into precise micro-movements inside your body. The robot cannot act independently — it only moves when and how the surgeon directs it.
-
Most robotic gynecologic procedures require four to five small incisions, each between 5mm and 12mm. These are closed with dissolvable stitches and typically heal to nearly invisible marks within a few months.
-
Clinical data shows robotic surgery has fewer complications, less blood loss, lower infection rates, and shorter hospital stays compared to open abdominal surgery. The overall surgical success rate for robotic procedures is 90-96%.
-
Many patients go home the same day. Some procedures, particularly Essure reversal and complex hysterectomies, may involve an overnight stay. Hospital stays rarely exceed one night for robotic gynecologic procedures.
-
Not all conditions require the robotic approach, but it's applicable to most gynecologic surgeries including tubal reversal, Essure reversal, hysterectomy, myomectomy, endometriosis excision, and ovarian cyst removal. Dr. Neef evaluates each patient individually to recommend the best approach.
-
Dr. Neef is the only physician in the DFW area who performs tubal reversal, Essure reversal, and hysterectomy using the Da Vinci robotic platform. He earned his medical degree from UT Houston and completed residency at UT Southwestern, and has been practicing in Burleson since 2008.
-
The incision marks are very small — about the size of a pencil eraser — and fade significantly over time. Most patients report that their scars are barely noticeable within a few months of surgery.
-
The Da Vinci system has been used for gynecologic procedures for over two decades. It's the most widely adopted surgical robotic platform in the world, with millions of procedures performed across multiple surgical specialties.
-
Coverage depends on the specific procedure and your insurance plan. Medically necessary procedures like hysterectomy are typically covered. Elective procedures like tubal reversal may not be. Dr. Neef's office can help verify your benefits and discuss financing options.
-
Dr. Neef practices at Texas Health Huguley Hospital Fort Worth South, Medical Office Building 3, located at 11797 South Freeway, Suite 358, Burleson, Texas 76028. The location offers easy access from Fort Worth, Arlington, Mansfield, Cleburne, and surrounding Johnson County communities.